Once a healthcare provider introduces the process of a bowel program, individuals are astounded at the procedure. I have yet to meet someone that is overjoyed in doing it. It is far from what people ever imagine they will do. Most have never envisioned it at all, so it is a totally new concept.
A very few people learn the steps to fecal removal and just go along with it. The vast majority of individuals take time to adapt to the process. Few begin a bowel program with little difficulty, and the process remains that way for years. Others do not seem to establish an effective process no matter what they do. Most fall somewhere in the middle. There are many variables and factors that affect the bowel program. Everyone’s internal functioning is also different; therefore, a bowel program can be a challenge.
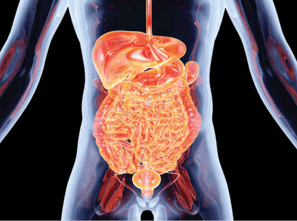
The basic bowel program follows one of two paths. For individuals with upper motor neuron (UMN) injury or typically injury at the cervical or thoracic level, the bowel is hyper-reflexive or spastic (tone). This can result in a small amount of stool being released as incontinence due to spasms, but the lower bowel's complete evacuation is not accomplished as stool remains in the bowel.
Those with lower motor neuron (LMN) injuries or those in the lumbar or sacral level have a flaccid bowel. The flaccid bowel does not respond well to stimulation. If the lower bowel becomes full of stool, the bowel will stretch to accommodate the overload. However, at times, a small amount of stool might be released as incontinence simply because there is no more room in the bowel, but a large amount of stool remains.
The goal of a bowel program is to remove stool from the body in a safe and efficient manner with no breakthrough incontinence.
The types of injuries lead to the foundation of the bowel program. Those with higher-level injuries will typically insert a suppository to stimulate the bowel, causing the lower bowel to be accelerated into action. Since higher-level injuries result in spasming, the internal rectal sphincter is general tightly closed. After the suppository is inserted, in about 10-15 minutes, digital stimulation with a well-lubricated, gloved finger is performed to relax the internal and external rectal sphincters, which allows stool to pass.
Those with lower-level injuries deal with a flaccid bowel that does not respond well to suppository or digital stimulation. For these individuals, manual removal of stool using a well-lubricated, gloved finger in the process.
Most people think of the bowel program as just being the process of elimination of waste from the body. But it is really a 24/7 process. These are other considerations of the total bowel program process.
Fluid: The bowel uses fluid to function. Fluid allows waste to be pushed through the bowel. If the stool becomes too hard too soon, it is difficult to move along in that long bowel. The stool can damage delicate bowel tissue and can be difficult or impossible to pass out of your body (impaction).
Water is the best option for keeping a moist stool. You can have other liquids but consider their effects. Alcohol causes dehydration that affects stool as well as the rest of your body. Caffeine can also dehydrate. Sugary drinks will cause the stool to move more quickly through the bowel. You can still enjoy these drinks. Just use them in moderation.
Fluid intake may be limited by your bladder program especially if you perform intermittent catheterization (IMC) where you cannot overfill your bladder too quickly. Often just an extra swallow or two can be instigated into your day. This is a small addition that will make a dramatic difference in your bowel function. Check with your healthcare provider to be sure adding fluid is right for you. Other healthcare issues require limiting fluid, such as cardiac diagnoses and some extreme cases of edema, among others. In this case, you can increase your fluids through a carefully managed diet as well as utilizing other management techniques that follow.
Diet: After SCI, the bowel tends to slow, which can make you feel full. That full feeling can lead to not wanting to eat. Changing your eating habits will have an influence on your bowel program. One of the top changes should be to reduce your intake of processed foods. Instead, eat fresh items, especially produce. This adds a tremendous amount of fiber to your diet.
There are certain foods that help move stool through the bowel. One of the top foods is beans. Beans have a pronounced effect on the bowel because of their fiber content. You can easily slip them into other dishes, such as adding them to salads, casseroles, soups, stews, or just as a side dish. Do not forget beans are popular as dips with fresh vegetables. Other fiber-rich foods are lentils, cooked potatoes, squash, seeds and nuts, bran, broccoli, cauliflower, cabbage, peas, and celery. Cereals are designed to have added fiber. Just be sure to check that the sugar content is not too high.
Sugar should be avoided. Individuals with spinal cord injury can develop a secondary complication of diabetes due to various factors, including lack of movement in their bodies. Limit sugar intake once the diabetic bowel senses sugar in any form. It tends to spontaneously speed its work which can lead to incontinence. You do not have to eliminate sugar and carbohydrates, again eat them in moderation or according to a diabetic food plan.
Fiber: Getting enough fiber into your diet is a challenge for just about everyone with or without a spinal cord injury. The daily fiber requirement for individuals under 50 years is 25 grams for women and 38 grams for men. After age 50, people tend to eat less on average, so the fiber requirement is lower, 21 grams for women and 30 grams for men. Most individuals with or without neurological issues struggle to reach these goals.
After SCI, and with age, your fiber requirement might be even higher due to that pesky slow bowel. Even though you might be able to consume the fiber requirement, it still might not be enough.
You can take fiber supplements that add a large amount of fiber. Several brands of fiber are sold under the title ‘fiber laxative’ as they do stimulate the bowel to move but not like a stimulant laxative that will make you incontinent. This form of fiber adds bulk to the bowel, making it easier to push stool along. The product is available in various brands, so if you do not like the taste or texture of one, you can try another. If you do not care for a powder added to water, you can try a wafer or other formulations. Check the package to assess the sugar content in the product. Sugar-free types are available, but I notice they are more costly. Being able to drink a large amount of water is critical to the use of these products. Fiber supplements can lead to gas and bloating. They are not the choice for everyone.
The products that add fiber are made of psyllium which is found online and in health food stores. The raw psyllium product does not have any added sugar or preservatives. You can sprinkle it on food or put it in your drink. You still need to drink plenty of water to activate it. Most say it tastes like nothing, but some individuals may or may not like the texture.
Gravity: Many individuals are taught to perform the bowel program in bed. This can reduce the incidence of hemorrhoids but makes a slower bowel program. A few individuals will need to continue to do this because of the inability to sit or due to the physical constraints of your home. If this is your situation, be sure to lay on your left side as physiologically, this will help with stool elimination.
The best position for a bowel program is sitting up. By sitting upright, you can take advantage of gravity to help the stool move down and out. Use of the toilet makes clean up easy. If you do not have a commode chair to assist in sitting and to cushion your seat, now is the time to have your healthcare professional order one for you. The commode chair can be placed over the toilet or used with a collection basin in a different room. If your bathroom is accessible, you can roll the commode chair right into the shower after your bowel program.
Sitting on the toilet or commode chair for extended periods of time does put a strain on the rectal area because it is not supported. The weight of your upper body is pressed on the rectum. Learn what your bowel elimination speed is. Many will insert the suppository, wait ten minutes for it to dissolve and activate your bowel, and then transfer it onto the toilet or commode chair. Others do not transfer until after the first digital stimulation—some need to transfer right away.
Activity: A huge part of bowel function is movement. This is often a missing process for individuals with SCI. But you can incorporate it into your life with huge benefits, just one being bowel function.
All your muscles interact and work together. When you move your legs either under your own power or if someone moves your legs for you, the muscles in the legs are exercised and as they move, they are affecting the muscles in your abdomen that surround your bowel. Upper body movement also affects the bowel as those muscles are connected to your abdomen as well.
People often overlook activity as a bowel movement process. You do not have to be working toward Olympic-level training. A gentle range of motion to the legs and lower body will affect your bowels. Even the movement of rolling side to side in bed or doing pressure releases positively affects the bowel.

