What Should My Urine Look Like?
Join Our Movement
What started as an idea has become a national movement. With your support, we can influence policy and inspire lasting change.
Become an Advocate
Trauma to your urethra or bladder is another cause of blood in your urine. If you catheterize without generously lubricating the catheter or have prostate issues, you might see pink or red in your urine from trauma. Be sure to lubricate the catheter well. Have your prostate checked. A Coudé catheter has a curved tip that slides around the prostate easier. This can be ordered for you by your healthcare professional. If the bleeding is not from trauma or there is frank blood in the urine is time for a call to your healthcare professional. Profuse bleeding is time for the emergency room.
Blue and green urine is usually from something you have eaten with blue or green food dye. Urine color affected by food dye is fairly rare but can happen. It quickly passes. The medications amitriptyline, indomethacin, cimetidine, and promethazine can turn urine green. Vivid blue urine can occur from dye used in certain medical tests and procedures. If you have one of these tests, you will be alerted that your urine will be blue. However, it may take the body a while to process the dye, so you might not see the blue color in your urine until after you are home. It is always a shock to see it, but you will remember it is from the test once you do. Most of the blue color is in the first toileting. A type of infection from the bacteria, pseudomonas, can change the color of urine to blue, green, or purple.
Urine should be transparent in that you should be able to see through it. It should be clear without any particles in it. Cloudy urine or a general look of haziness can be a sign of urinary tract infection or dehydration. It can also indicate a kidney condition is present. Pneumaturia is urine that is cloudy with foam. It could be nothing or an indication of Crohn’s disease or diverticulitis. Further testing is needed.
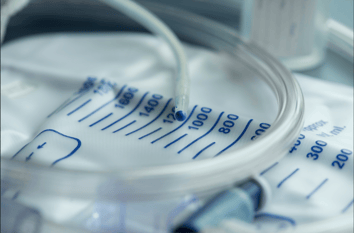
Sediment is sometimes seen in urine, especially in individuals with paralysis. Sediment looks like tiny white, reddish, and brown particles that settle in a urine collection device. A small amount of sediment can be normal in urine, but it is such a small amount that it is typically not seen. Sediment is not seen if you use the toilet because most toilets are white, as is most sediment. Water in the bowel also dilutes the concentration of urine, so the sediment is not visualized. Usually, sediment is only seen in a collection device by individuals who catheterize. Sediment can be present consistently or intermittently.
Often people think sediment is an indication of a urinary tract infection, which is often is but not always. Sediment in the urine can result from urinary tract infection, kidney infection, bladder infection, kidney stones, vaginal bacteria, yeast infections in men and women, prostatitis, and parasites. Sediment has been related to bone mineral loss after spinal cord injury. It is also due to pregnancy and retrograde ejaculation. If you have increased sediment in your urine, you will need to have a urine test.
Urine can have an extremely strong odor. Most often, the smell is from a high concentration of waste products produced by your kidneys. Eating asparagus, foods high in protein and vitamin B6, are culprits for smelly urine. Pregnant women occasionally have a strong odor to their urine. Dehydration, urinary tract infection, kidney infection, kidney stones, and liver disease can also affect the smell of your urine. Diabetes is a particular culprit for odor in urine. An increase in ketones in the bloodstream can create an ammonia smell. As diabetes can be a secondary complication to paralysis due to lack of muscle metabolism, a new ammonia smell or increase can be the first sign of diabetes or an indicator that your diabetic medication needs adjusting.
This is a lot of information about what changes in your urine can mean. It does not necessarily mean that you have any of these conditions, but it is good to be aware. Relying on visual inspection of urine is just one clue to your urinary health. If your urine changes, you may need a urinalysis test at the minimum. Urinalysis will detect issues in your urine that you cannot see. Your healthcare professional will direct you by the results of your test. Early intervention, especially in urinary conditions, allow for faster and more efficient treatment. Nurse Linda
Pediatric Consideration:
Urine visual inspection is a way to monitor your child’s urinary health. Children cannot always express issues in adult ways. Cues from their behavior and looking at things like urine can help discover issues, establish their normal, and be able to obtain early intervention.
There is one other color change in urine that might be seen in children. A very rare inherited disorder, familial benign hypercalcemia or hypocalciuric hypercalcemia, results in blue urine. A biological parent or someone in their family will have this condition, so typically, families are aware of it. I mention it in pediatrics because that is when it is usually discovered. The child has ‘blue diaper syndrome’ because, in some cases, urine is blue in the diaper. Not all individuals with this condition have this symptom.
Individuals who have familial benign hypercalcemia have a high concentration of calcium in the blood and urine. The parathyroid gland can be affected. Most individuals have no symptoms. Individuals have normal lifespans, normal bone density and do not have increases in bone fractures. In some incidences, individuals may have a tendency for gallstones, may have fatigue, concentration issues, and thirst. The pancreas can be affected, and extra calcium might affect the joints. Treatment is usually unnecessary but can be by symptom if needed.